You're not alone
You're not alone

Wether you’re exploring symptoms or were recently diagnosed, I’ve consolidated the resources that I wish were readily available for me when I began my journey to remission. The internet can be overwhelming, doctors can be vague and the confusion can become debilitating. Read about the first steps to diagnosis and my journey with chemo, radiation and fertility below!
chemotherapy / radiation / fertility
Chemotherapy
Multiple doctors were pushing, calling, and begging me to do PCV chemo & my response was F-THAT.
I no longer picked up their calls and got new doctors.

I decided to move forward with an option called Temodar (Temozolomide), which is an oral alternative to PCV chemo. Its generally taken once a month for a 5 day period. During this treatment I go in twice a month for blood tests to ensure everything is trending normal. My doctor recommended getting a blood test 3 weeks after I take Temodar, when my body is at its weakest, then again before starting chemo again (week 4) to ensure my white blood cell count, hemoglobin, and platelet numbers were at safe levels. Every time I got a blood test there were flags that popped up but don’t freak out! This is completely normal when taking a form of chemotherapy and doctors will notify you if anything is amiss.
Dr. Hattangadi-Gluth and Dr. Piccioni both stated that young women are typically affected more severely by chemo causing their white blood cell and platelet count to drop more dramatically. My white blood cell count didn’t drop too sharply, but my platelets were severely affected to a point where my doctor asked me to stay near a hospital in case I needed a platelet transfusion. I didn’t end up needing one and they lowered my dose of Temodar after just to be safe. This is why regular blood testing is important during this stage of treatment, and why it is so important to be in constant communication with your doctor.
That being said, any form of chemo is not fun. I felt like I had a flu and hangover at the same time for each week I was taking the Temodar—that being said, it definitely could have been worse. My doctors made sure I was as comfortable as possible and I could contact them at any time. I was stocked up with water, electrolytes, soup, and tons of movies and books. It kind of just became my “lazy week” and then I was back to normal afterwards during my off weeks. Proper nutrition and vitamin intake during this time seemed to help a lot, and is something I highly recommend taking a close look at—often treatment centers have a nutritionist on site to consult.
The timespan for how long I would be doing chemotherapy was essentially up to how my body reacted—my blood and well-being was closely monitored. When I started Temodar, the goal was a minimum of 6 months, a max of 12 and to aim for 9 months. I am currently in my 6th month and so far so good.
I feel like it is also important to note that you don’t have to be on a strict schedule for the Temodar—of course I was as strict as I could possibly be—but I did turn 30 this year and the chemo start date was going to be a couple days before my 30th birthday. I asked Dr. Piccioni if I could move it back by a few days and he said absolutely and to enjoy a glass of Champagne.
FAQ
-
Yes. Multiple doctors stated that PCV was the “gold standard” for chemotherapy for brain tumors whereas other doctors I spoke with stated that Temodar (Temozolomide) was the gold standard.
The reason why doctors reccomend PCV chemo is because it has been around longer. Theres still clinical trials going on (which have been going on for 10+ years) to see which works better. So, no one knows.
PCV is infusion chemo which is much harsher on your body and will make you immunocompromised and potentially infertile.
Temodar is very mild, you can take it during radiation, you don’t lose your hair, or become immunocompromised, and some people have been able to conceive children after taking Temodar.
-
I first started taking 140mg of Temo nightly conjunctively with radiation. My thoughts were “lets just get this sh*t done.” I didn’t feel too bad on it. Nauseous some days and other days were fine. It did curb my appetite quite a bit and I was pretty turned off by meat/fried or heavy food for about 2 months.
When I started doing the maintenance Temo at 265mg I felt a little worse but not bad all things considered. It sort of felt like a moderate/bad hangover for 5 days then I was super tired for about a week after.
Everyone has a different experience though! So I would love to hear your experience on Temo as well.
-
After I found out about the side effects it can have on your body, no. Although some doctors were VERY convincing and pushy about it. They even had their nurses calling me to tell me to do it.
-
Everyone’s doctors may have a different opinion but my doctor wants me to do at least 6 months of the 5 days a month regimen. They are going to monitor my white blood cell count and platelet count twice a month to see how my body is handling it. They said the longer I do it, the least likely it’ll be that it comes back.
I am still currently taking the Temodar.
-
Yes. They prescribed me Zofran to take 1 hour before taking the Temodar. Zofran is great at counteracting nausea.
They also prescribed me Miralax because the Temo and Zofran can make you constipated.
Finally, I was prescribed Bactrim. A combination of two potent antibiotics used to treat pneumonia, bronchitis, UTI’s, respiratory and intestinal infections. As recommended by my radiation oncologist, I did not take the Bactrim because I was not at risk for any of those infections to occur.
My radiation oncologist also told me that I did not need the Bactrim.
-
I did notice that the more water I drank the better I felt so, I would try to drink around a gallon of water over the course of the day and the days leading up to taking the Temodar.
Also, it is EXTREMELY important that you are going number 2… the worse your constipation gets the worse you feel… I found this out the hard way. Temodar makes you constipated, Zofran makes you constipated–heed my warning.


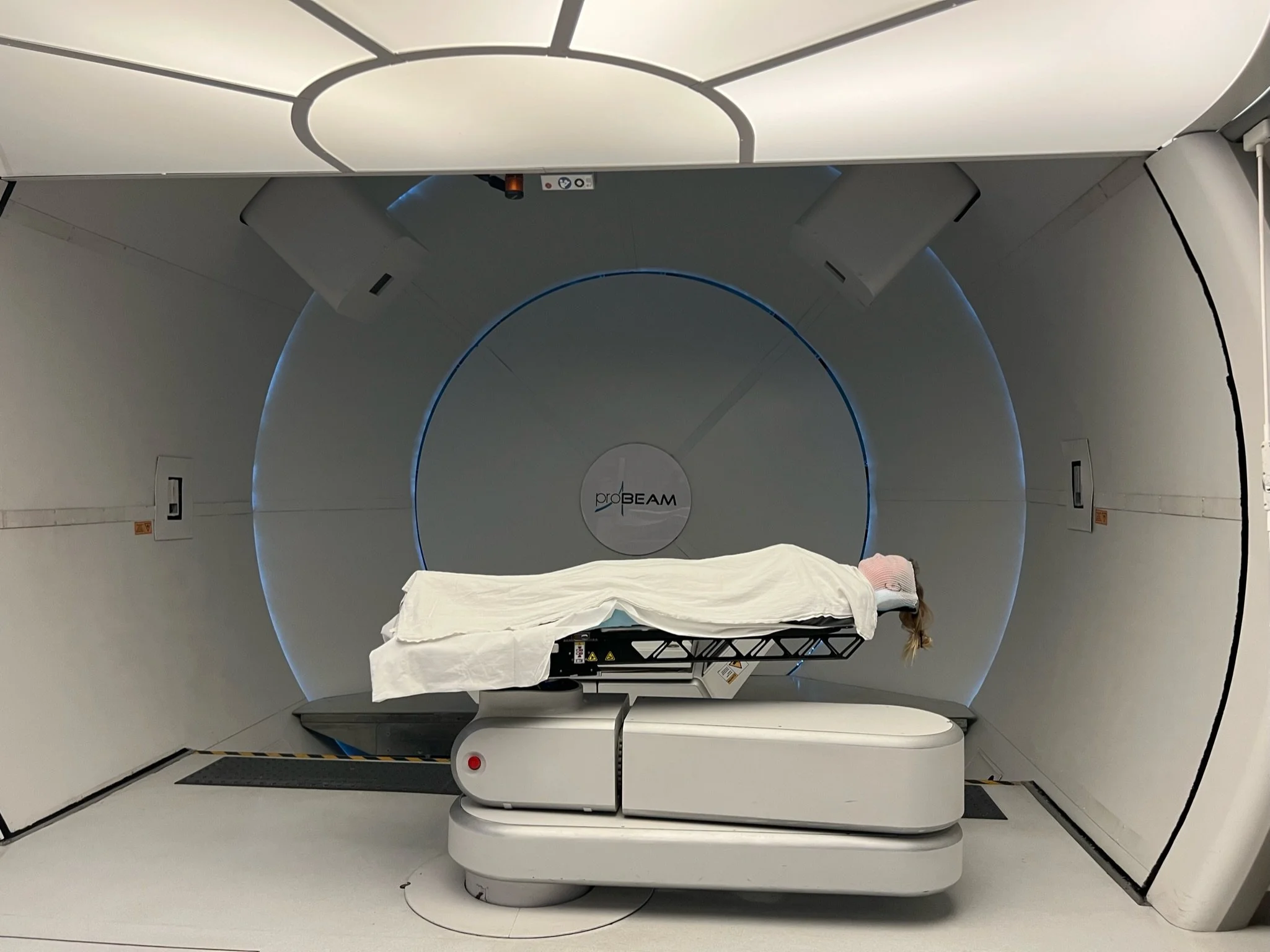
Radiation
My first radiation information appointment was with Ridley Tree Cancer Center in Santa Barbara with Dr. Suh. He was very kind and informative of different radiation options. He stated that because I was young he would recommend me to go to a Proton Radiation Center instead of Photon Radiation, which is what they had at Ridley Tree. With any type of radiation there is a small risk of alternative cancers appearing later in life. Proton radiation is the lowest exposure of radiation so that is why he told me I should look into it.
The nearest Proton Radiation Center was with California Protons Cancer Therapy Center in San Diego. The Proton Therapy Center is affiliated with UCSD and Rady’s Children Hospital. So, I called to set up a Zoom appointment with Dr. Hattangadi-Gluth later that week. I sent all of my information down to the center for Dr. Hattangadi-Gluth to review prior to our appointment. She was fantastic and I instantly liked her knowledge, energy, and positivity and I knew that I wanted to go to San Diego for the proton treatment after the call. I set up an intake appointment to be able to start treatment within the next month. I highly recommend getting treatment here if you can!
FAQ
-
After I was referred to a radiation oncologist, he recommended I go to California Proton Therapy Center for their proton radiation. He made the referral and I spoke with their radiation oncologist and she educated me on the difference of proton vs. photon radiation. I was very intrigued and sounded like the right fit for me so I made an appointment for a start date in January of 2023.
For more information on Proton Radiation please go to the link below!
https://my.californiaprotons.com/
-
Proton radiation was invented for children and young adults. With its pin point precision, proton radiation spares healthy tissue much more than photon radiation which decreases your risk of getting other cancers in the future.
That being said, photon radiation is still a great choice. My doctor recommended if my insurance did not approve me for the proton radiation that I shouldn’t spend precious time fighting my insurance, but just do the photon radiation instead.
-
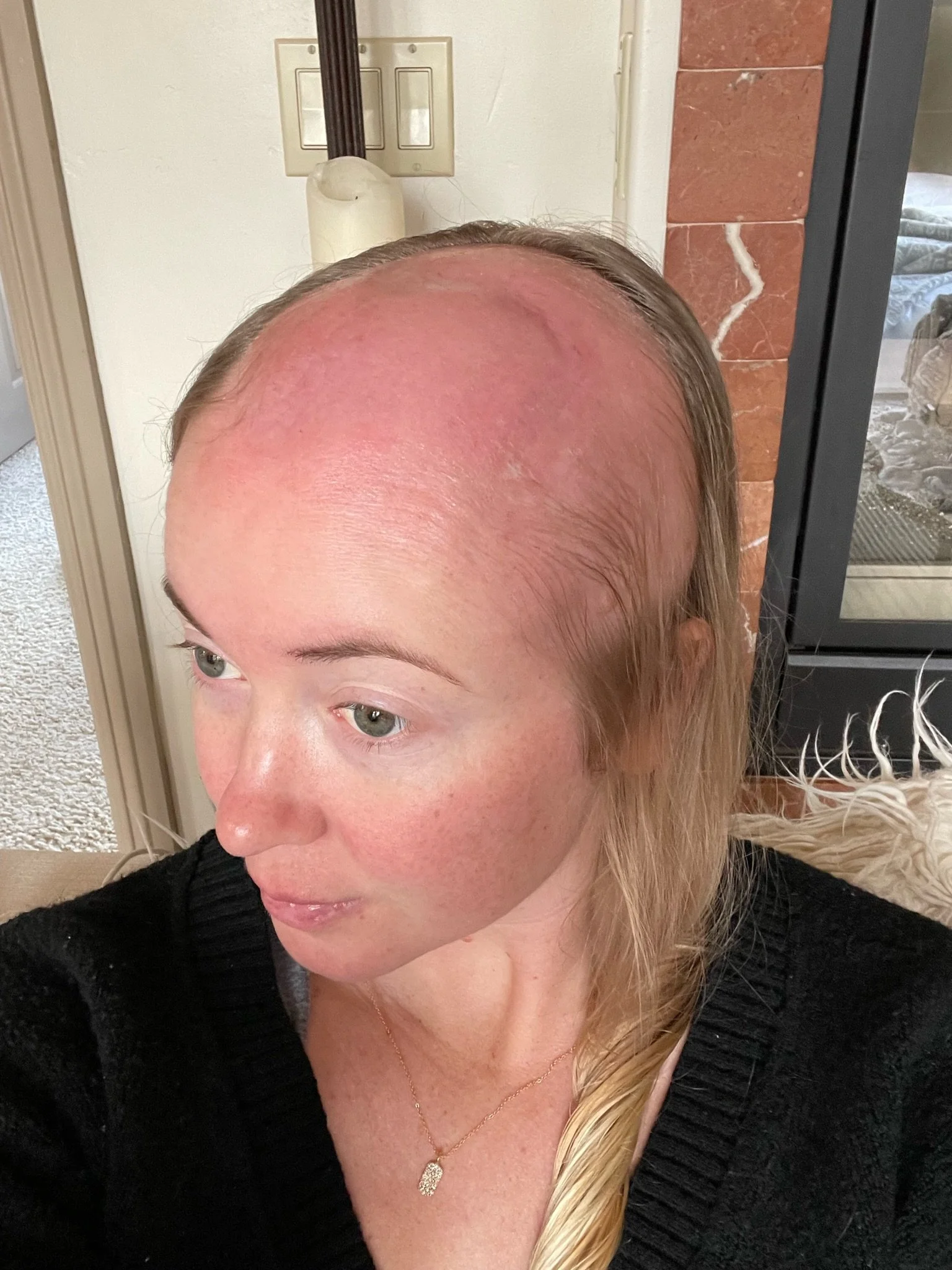
My scalp just got pretty sunburned, dry and itchy. Then I lost about 99% of my hair in the 3rd week. It took about 2 days for it to all come out in the radiation area. My doctor did say that hair follicles are much more susceptible to radiation and you can lose a larger portion of hair than whats actually being treated—like what happened to me.
Otherwise, the fatigue wasn’t too bad. I took naps during the day but it was mostly cause I was bored and wasn’t at my own home.
-
Nope! I was told its like someone shining a flashlight on your head. According to the nurses in the room you cant even see a beam.
-
I did 33 sessions. Each session takes about 20 minutes. Thats the standard amount of sessions and you go in everyday during the week M-F. They are closed on the weekends.
They let you choose the music in your sessions too!!
-
They moulded a custom mask over my face and put it on every time I was in my appointment—not until I was laying on the table though. It clips into a custom pillow they mould with the mask which clips into the table.
It was fairly claustrophobic in the mask but you can still breathe and see out of it. Its just flush against your skin and sort of smashes your lips and eyelids down. Not too terribly though. I couldn’t stop laughing when I saw a picture of me in the mask!
-
Yes—although they took a LONG time making their decision.
But, I asked the out of pocket cost regardless so I could make an appointment.
Out of pocket cost is around $20,000.
-
The facility and staff were so great. I couldn’t recommend them enough. It didn’t feel like a hospital which was a big plus. Everyone cried and gave me a medal on my last day - so sweet!
Fertility



Unbeknownst to me, cancer treatment effects fertility - go figure.
I was referred to an oncologist 2 weeks after the brain surgery when I was informed of the possible side effects of chemotherapy on fertility. PCV and Temodar would most likely make me infertile so he suggested seeing a fertility doctor to talk about my options. At first I refused because I wasn’t even sure I wanted kids, I hadn’t thought about it—at all.
It took me 2 weeks to change my mind so I made an appointment to see the only fertility doctor that had sponsorship opportunities for cancer patients in my city. My boyfriend and I met with him over a video-call and he was very kind and informative about all of my options. After the call, I decided to go forward with the egg retrieval. I didn’t want the option of having kids to be taken away from me if I later changed my mind because if I can’t control cancer I might as well be able to control this.
I was supposed to start radiation as soon as my head fully healed so I had a very small window to do the egg retrieval and only enough time for one attempt. If they didn’t get enough then too bad. I went into the office the next day to start the two-week process. LiveStrong and Heart Beat foundation sponsored my hormones and the rest I had to pay out of pocket.
Typically, the egg retrieval is timed with your period cycle but due to my radiation schedule, we started right away. One blood test, a really fun hoo-ha ultrasound, some paper work and a lesson on how to reconjugate vials later I was instructed to start the injections that night.
FAQ
-
There were a few of fertility options. I could freeze eggs, embryos, or risk it and try to conceive later in life. Which is possible for some people to do. I just didn’t want to take that chance.
-
No. Which is honestly ridiculous. Even if a woman who doesn’t have cancer wants to do the process of egg retrieval it should be covered by health insurance.
Fortunately, my hormones were covered by LiveStrong and HeartBeat which was about half the cost.
As well as the first 3 years of cryopreservation for free.
-
Painful, no. Uncomfortable, yes. The weeks leading up to the egg retrieval were a little rough. I felt like I was waddling around and very hormonal/emotional. But, I was getting injected with a lot more of my naturally occurring hormones so it makes sense.
After the egg retrieval I got OHSS (ovarian hyper-stimulation syndrome) which was very painful, but is very rare. Also trying to go to the bathroom was the worst thing ever.
-
An egg or an embryo can remain in a cryopreservation tank for days, weeks, or years depending on a person's needs.
-
Santa Barbara Fertility Center. Dr. Renee Allen was my fertility doctor.
Making brain tumors less scary.
Resources, insight & encouragement from a fighter herself
